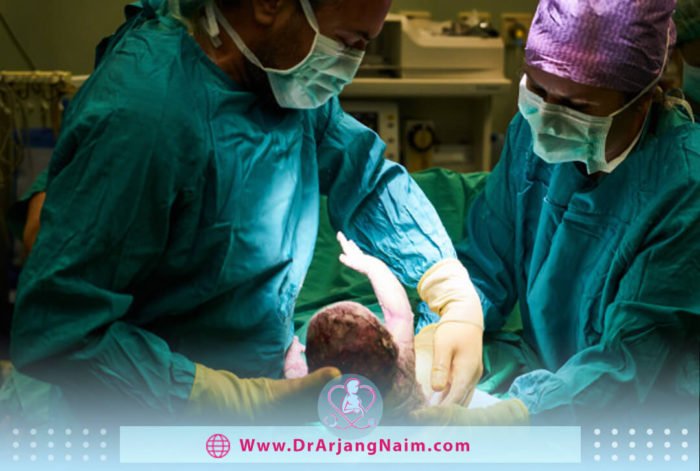
C-section is one of the delivery methods in which the mother’s abdomen and uterus are cut, and the fetus is removed. Cesarean section is not a good alternative to natural childbirth due to its complications for the mother and fetus. It is useful and necessary when the mother cannot have a normal delivery because a normal delivery may endanger the mother and fetus‘s health.
Cesarean section is a procedure that delivers the baby through the abdomen. The doctor makes a 4-6 inch incision in the skin above the pubic bone and removes the underlying tissue. It then makes an incision through the lower part of the uterus, just above the bladder, and removes the baby. Generally, regional anesthesia is performed during a C-section, and the mother is usually awake; a veil is placed over her chest to prevent her from observing surgery. Surgery usually takes between 25 and 60 minutes.
How to perform a cesarean section
Before the cesarean section, angiography is performed through an angiocatheter in one of the arteries to give the mother fluids and, if necessary, medication. The abdomen is then anesthetized with spinal anesthesia, epidural anesthesia, or both. General anesthesia, which quickly causes the mother to fall asleep, is performed only in emergencies. In most cases, the mother can be conscious during C-section due to local anesthesia and hug the baby after birth.
After the mother is anesthetized, the doctor makes a transverse incision in the upper part of the genitals. The doctor removes the baby from the uterus after the incision. After removing the baby, the doctor removes the placenta from the uterus and finally sutures the surgical incision. Due to the possibility of material returning from the esophagus to the airways to the gastrointestinal tract during surgery, fasting is at least eight hours before the scheduled cesarean section.
Types of C-section
- Types of the cesarean sections include:
Scheduled C-section: In this case, the mother and the doctor decide it is safe for the mother and baby to have a cesarean delivery. The doctor gives an estimated date for surgery. - Unplanned C-section: In this case, the mother intends to have a vaginal delivery, but shortly before delivery, the doctor decides that cesarean section is a better method for both mother and baby. This decision can be made in weeks, days, or even hours before delivery. With an unplanned cesarean section, there is no emergency.
- Emergency C-section: This happens when labor needs to be done quickly so that the mother and baby’s health is not endangered.
Two main reasons for a C-Section
Cesarean section can have different causes. Some of these cases relate to the mother’s health, meaning that if the doctor determines that the mother cannot continue the pregnancy or that a normal delivery endangers her health, she can have a C-section. There is another category of reasons related to the fetus’s health, in which case the obstetrician determines that to maintain the fetus’s health, they should use the cesarean section method for delivery. The most important reasons for having a cesarean include the following:
- Cervix doesn’t dilate
- No reassuring fetal heart rate tracing
Cervix doesn’t dilate
When labor does not progress, the cervix does not dilate, and the baby does not descend.
Cephalopelvic Disproportion (CPD)
It may sometimes be suspected before delivery, in late pregnancy. It happens if the doctor thinks the mother has a narrow pelvis or a prominent sacrum, which may make labor slower or more difficult. However, a pelvic assessment alone is not an accurate way to predict whether vaginal delivery is possible. In some cases, vaginal delivery is possible even if the pelvis is not in good shape. In vaginal delivery, the pelvis’s shape and the interaction between the baby and the pelvis are important.
If CPD is suspected, but the baby’s head has engaged, vaginal delivery can still be performed. But if the head is not engaged at the end of labor, a scheduled cesarean section may be performed.
Inefficient Contractions
If labor is not progressing because the cervix is slowly dilating, your doctor will assess the frequency of contractions. The tighter the contraction, the more likely it is to be effective. If the contractions are longer than allowed, and their strength shows that they are unlikely to be effective, they may use one or two methods to speed up labor, which is called augmenting delivery.
The first step is to artificially rupture a membrane that has not already ruptured, a process called ARM. If ARM does not work, oxytocin may be given to increase the strength and frequency of contractions. Initially, a small dose is given and then increased until three or four moderate to severe contractions occur every 10 minutes. A C-section may be recommended if labor does not progress within a few hours of starting the medication.
Posterior Presentation
The baby’s best position during childbirth is an occipital-anterior position with the head’s back facing the front. If the head’s back faces back, it can make it difficult for the baby to rotate and move down the birth canal and prolong labor. If the baby cannot turn, forceps may be used to assist with delivery. In cases where the baby is not in good condition, the obstetrician may recommend a cesarean delivery.
No reassuring fetal heart rate tracing
It is important to monitor the fetal heart rate to ensure the baby is doing well in the third trimester of pregnancy and during delivery. The fetal heart rate during late pregnancy and delivery is between 110 and 160 beats per minute. Doctors may use internal or external devices to monitor the fetus’ heartbeat. Heart rate is often measured using an ultrasound device.
When examining the fetal heart rate, the doctor pays attention to its decelerations and acceleration. Any change in heart rate may be a sign that the baby or mother is in physical danger. Such signs of trouble may force the doctor to take immediate action for cesarean delivery.
Other medical reasons for C- section
Other reasons why obstetricians use C- section includes:
- Birth defects: To reduce labor complications, doctors decide to deliver babies diagnosed with certain congenital defects, such as excess fluid in the brain or congenital heart disease, by cesarean section to reduce labor complications.
- Chronic health condition: If women live with certain chronic health conditions, such as high blood pressure, heart disease, or gestational diabetes, their doctor may decide to have a cesarean section. Doctors also recommend a cesarean section if the mother has HIV, genital herpes, or any other infection that can be passed on to the baby through vaginal delivery.
- Placenta issues: If the placenta does not have the right nest, the mother will have placental abruption. Placental abnormalities make it difficult to have a normal delivery. To protect the health of the mother and fetus, the doctor will recommend a cesarean section.
- Carrying multiples: Multiple pregnancies can have various risks during pregnancy that can lead to prolonged labor, putting the mother in a difficult position. One or more babies may also be in an abnormal position. However, a cesarean section is often the safest route for delivery.
- Previous C-section: Having a cesarean delivery before or other surgeries on the uterus increases the risks of a normal delivery complication. In some cases, even with a previous cesarean section, a normal delivery can be safely performed, which is called VBAC. The doctor will check the condition to make sure there is a possibility of vaginal birth after a cesarean section.
Risks of C-section
Cesarean section, like any other surgery, has risks. Some of these risks are related to the mother, and some to the fetus.
Risks for the fetus
In some cases, cesarean delivery may pose risks to the fetus. These risks include:
- Breathing problems: Babies born by scheduled cesarean section are more likely to develop transient tachypnea. Tachypnea is a respiratory problem characterized by abnormally rapid breathing during the first few days after birth.
- Surgical injury: In rare cases, there may be a chance of harm to the child, just accidental nicks and scrapes.
Risks for the mother
Risks to the mother include:
- Infection: After a C-section, the lining of the uterus may become infected.
- Reactions to anesthesia: The mother may have an adverse reaction to anesthesia.
- Postpartum hemorrhage: C-sections may cause severe bleeding during and after delivery.
- Surgical injury: Although rare, surgical injuries to the bladder or bowel can occur during a C-section.
- Blood clots: C-sections may increase the risk of blood clots forming inside the veins, especially in the legs or pelvic organs.
- Increased risks during future pregnancies: Cesarean section is riskier for serious complications than vaginal delivery in the next pregnancy. The higher the number of cesarean deliveries, the greater the risk of placenta previa and the condition that the placenta attaches abnormally to the uterine wall. The risk of uterine rupture along the scar line is also higher if VBAC is performed.
After the procedure
After a cesarean section, the mother usually stays in the hospital for a few days. The health care provider outlines options for pain relief. When the effects of anesthesia subside, the nurse encourages the mother to drink plenty of fluids and walk, preventing constipation and deep vein thrombosis. The health care team monitors the incision for signs of infection. If a bladder catheter is used, it will be removed as soon as possible.
As soon as the mother feels satisfied, she can start breastfeeding. A nurse or breastfeeding counselor teaches the mother how to position herself and start breastfeeding.
Contact the doctor after discharge from the hospital if have any of the following symptoms:
- Breast pain accompanied by a fever
- Pain when urinating
- Foul-smelling vaginal discharge
- Bleeding with large clots
- Signs of infection, for example, fever over 100 °F, swelling, redness, or discharge from the incision
C-section recovery tips

After the mother goes home, she should provide as much comfort as possible to rest. Everything needed for the mother and child is available. In the first few weeks, do not lift anything heavier than the baby and seek help from others if possible. Use a warming pad, ibuprofen, acetaminophen, or other painkillers your doctor recommends to relieve the pain. To prevent infection, abstain from sex for six weeks after cesarean section. Also, it is best not to drive while taking painkillers to reduce pain.
Keep the incision clean and ask the doctor about its care. Wear loose clothing and pants that do not irritate the abdomen. Itching and stretching around the incision and numbness is normal and will disappear shortly. The post-cesarean diet should be carefully adjusted. The diet must combine the main food groups with meeting the mother’s body’s need for essential nutrients.
Shortly after giving birth, the mother may experience severe mood swings, loss of appetite, fatigue, and depression. If the mother feels depressed, talk to a counselor about her symptoms.
The bottom line
As it turns out, normal delivery is better than a vaginal delivery, but in some cases, cesarean delivery is performed according to the mother and baby’s condition. Keep in mind that in C-section, in addition to the pain at the incision site, the mother will experience almost the same symptoms as in vaginal delivery, such as fatigue, slight contractions, bleeding or discharge after delivery, and breast engorgement. Therefore, the mother must have the necessary care after childbirth to have a good time with her baby.
Dr. Arjang Naim, MD makes regular appointments throughout the pregnancy to check on the mother and baby’s condition, set at shorter intervals in the last month of pregnancy. The mother and baby’s condition is thoroughly examined to select the best delivery method during which there are the least risk and complications for the mother and baby.
Additional questions
- How long will C-section pain last?
After a cesarean section, you may have a little pain in the lower abdomen and need painkillers for 1 to 2 weeks. Vaginal bleeding can continue for several weeks.
- How many stitches are in a C-section?
At the beginning of the cesarean section, six layers of the abdominal wall and the uterus are opened separately. After delivery, the uterus is closed with two layers of stitches.
- What are the cervix and its function?
The cervix is the part of the female reproductive system that connects the vagina to the uterus. It plays an important role in the menstrual cycle, fertility, pregnancy, and childbirth.
- Which baby position is best for normal delivery?
The best position for childbirth is the anterior position. Anterior position means the baby’s head enters the pelvis facing the back. This is the ideal and most common position for birth.
- Which week is best for cesarean delivery?
Experts recommend that a planned cesarean delivery be performed from the 39th week onwards to complete the maturation of the fetus.
References
https://www.webmd.com/baby/risks-of-a-c-section
https://www.webmd.com/baby/emergency-c-section#1
https://www.healthline.com/health/pregnancy/c-section-reasons#Takeaway-
https://www.healthline.com/health/pregnancy/abnormal-fetal-heart-tracings#decelerations
https://www.healthline.com/health/pregnancy/emergency-c-section#why-they-happen
https://www.whattoexpect.com/pregnancy/c-section/
https://www.healthline.com/health/c-section#follow-up
https://www.whattoexpect.com/pregnancy/c-section/