Antiphospholipid syndrome is when the body’s immune system mistakenly makes antibodies that attack the body’s tissues. These antibodies can cause blood clots in the arteries and veins.
Blood clots can form in the legs, lungs, and other organs, such as the kidneys and spleen. Clots can lead to heart attack, stroke, and other conditions. During pregnancy, antiphospholipid syndrome can also lead to miscarriage and stillbirth. Some people with this syndrome have no signs or symptoms. There is no cure for this rare condition, but medications can reduce the risk of blood clots and miscarriage.
Symptoms
Signs and symptoms of antiphospholipid syndrome can include:
- Blood clots in the legs (DVT): Symptoms of deep vein thrombosis include pain, swelling, and redness. These clots can travel to the lungs (pulmonary embolism).
- Repeated miscarriages or stillbirths: Other complications of pregnancy include high blood pressure (pre-eclampsia) and premature birth.
- Stroke: A stroke can occur in a young person who has antiphospholipid syndrome but no known risk factors for cardiovascular disease.
- Transient ischemic attack (TIA): Similar to a stroke, a transient ischemic attack usually lasts only a few minutes and causes no permanent damage.
- Rash: Some people develop a red rash with a lace-like pattern.
Less common signs and symptoms include:
- Neurological symptoms of chronic headaches, including migraines, dementia, and seizures, can occur when a blood clot blocks blood flow to parts of the brain.
- Cardiovascular disease. Antiphospholipid syndrome can damage the heart valves.
- Low blood platelet count (thrombocytopenia). This reduction in blood cells needed for clotting can cause bleeding, especially from the nose and gums. Bleeding on the skin appears as small red spots.
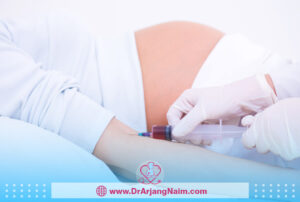
How is antiphospholipid syndrome diagnosed?
Antiphospholipid syndrome (APS) is diagnosed based on a combination of clinical criteria and laboratory tests. The diagnosis typically involves confirming the presence of specific antibodies associated with the condition in the blood and the occurrence of clinical symptoms or events characteristic of the syndrome.
Clinical criteria
Clinical criteria include:
- Thrombosis: One or more clinical episodes of arterial, venous, or small vessel thrombosis occurring in any tissue or organ. Thrombosis must be confirmed by imaging Doppler studies or histopathology, with the exception of superficial venous thrombosis.
- Pregnancy Morbidity: One or more unexplained deaths of a morphologically normal fetus at or beyond the 10th week of gestation.
One or more premature births of a morphologically normal neonate before the 34th week of gestation due to eclampsia, severe preeclampsia, or placental insufficiency.
Three or more unexplained consecutive spontaneous miscarriages before the 10th week of gestation, with maternal anatomic or hormonal abnormalities and maternal and paternal chromosomal causes excluded.
Laboratory criteria
There are laboratory criteria for diagnosis.
Antiphospholipid antibodies
The presence of antiphospholipid antibodies is required for the diagnosis. These antibodies must be detected on two or more occasions at least 12 weeks apart and may include:
- Anticardiolipin antibodies (IgG or IgM): Moderate to high levels measured by a standardized enzyme-linked immunosorbent assay (ELISA).
- Lupus anticoagulant: Presence detected according to the guidelines of the International Society on Thrombosis and Haemostasis.
- Anti-β2 glycoprotein I antibodies (IgG or IgM): Again, moderate to high levels measured by standardized ELISA.
Additional considerations
- Temporal Stability: Antibodies should be tested twice, at least 12 weeks apart, to confirm persistence. This is important for diagnosis as transient positivity can occur in various conditions, including infections.
- Rule Out Other Causes: Other potential causes of thrombosis and pregnancy loss, such as genetic thrombophilias, hormonal factors, and anatomical abnormalities, must also be excluded.
Diagnostic process
- History and Physical Examination: Document the patient’s medical history, including any instances of thrombosis or pregnancy complications.
- Blood Tests: Initial testing for anticardiolipin antibodies, lupus anticoagulant, and anti-β2 glycoprotein antibodies. If positive, these tests are repeated 12 weeks later.
- Imaging Studies: These may be performed to confirm thrombosis.

Risk factors
Antiphospholipid syndrome is more common in women than men. Another autoimmune disease, such as lupus, increases the risk of developing antiphospholipid syndrome.
It is possible to have antibodies associated with antiphospholipid syndrome without causing signs or symptoms. However, having these antibodies increases your risk of blood clots, especially if you:
- Pregnancy
- Being immobile for a while (such as resting in bed or sitting during a long flight)
- Cigarettes
- Surgery
- Menopause Use of estrogen therapy or oral contraceptives during menopause
- High cholesterol and triglyceride levels
How is antiphospholipid syndrome treated in pregnancy?
Treatment of antiphospholipid syndrome (APS) during pregnancy is important to reduce the risk of complications such as pregnancy loss, preeclampsia, intrauterine growth restriction, and preterm delivery. The primary goal of treatment is to prevent thrombotic events and improve pregnancy outcomes. This approach generally involves medications that help manage blood clotting and close monitoring of the mother and fetus.
Low-dose aspirin
- Purpose: To prevent blood clot formation and improve uterine placental blood flow.
- Diet: Low-dose aspirin is usually started before pregnancy or in early pregnancy.
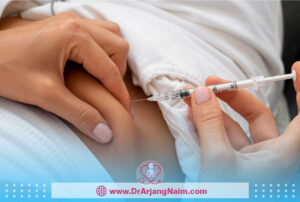
Heparin
- Types: Unfractionated heparin or low-molecular-weight heparin are used, with low-molecular-weight heparin being preferred due to its better safety profile, longer half-life, and lower risk of osteoporosis and thrombocytopenia caused by heparin.
- Purpose: To prevent thrombosis by thinning the blood. Heparins are safe in pregnancy because they do not cross the placenta.
- Diet: The dose and type are determined based on the patient’s weight, history of thrombosis, and risk assessment.
Monitoring
- Pregnancy monitoring: Frequent obstetric and gynecological visits are recommended to monitor the fetus’s health and the diet’s effectiveness. This includes regular ultrasounds to assess fetal growth and health and Doppler ultrasounds to monitor placental blood flow.
- Blood tests: Monitor platelet counts and anti-Xa levels to ensure therapeutic anticoagulation levels and adjust dosage as necessary.
Additional considerations
- Timing of Delivery: The time and manner of delivery is often carefully planned. Labor may be induced to control the timing of labor in a monitored setting.
- Transitional anticoagulants: Women may need to change the dose and type of heparin as they approach delivery.
Postpartum care
- Postpartum anticoagulation: Anticoagulation is usually continued for at least 6-12 weeks after delivery because the risk of thrombosis remains high.
- Breastfeeding: Breastfeeding is generally considered safe while using heparin.
Special cases
Women with a history of thrombosis or those with a positive lupus anticoagulant test may require a more aggressive anticoagulation strategy. Additional treatments may be considered based on individual risk factors and any other co-existing conditions.
Collaborative care
Management of APS during pregnancy involves a multidisciplinary team approach, including obstetricians and gynecologists specializing in high-risk pregnancies, hematologists, and sometimes rheumatologists. This collaboration is necessary to adapt the treatment plan to the individual’s needs and to respond to changes in her condition during pregnancy.
Complications
This disease can cause serious problems during pregnancy for both mother and child. Women who have this condition are also at risk for other problems. Some of these are:
- Stroke
- High blood pressure in pregnancy
- Stillbirth
- Blood clots
- Multiple miscarriages
- Poor fetal growth
- Preterm birth
Living with antiphospholipid syndrome
Antiphospholipid syndrome is a lifelong condition that requires treatment. This reduces the risk of blood clots. It also reduces the risk of complications such as stroke and miscarriage.
Medication can reduce the risk of blood clots, but they can still occur. It’s important to follow your healthcare provider’s care plan and get tested as often as he or she recommends. Support groups can help you meet other people with your condition. Ask your healthcare provider about support groups in your area.
How to reduce the risk of blood clots in pregnancy?
Along with treatment, there are things you can do to reduce your risk of blood clots and increase your chances of a healthy pregnancy and baby. This includes:
- Not smoking
- Eat a healthy and balanced diet
- Exercise
- Management of weight gain during pregnancy
- Knowing the signs and symptoms of blood clots
The bottom line
In managing antiphospholipid syndrome (APS) during pregnancy, early intervention with low-dose aspirin and heparin is essential to prevent complications like thrombosis and pregnancy loss. Close monitoring through regular obstetric visits and blood tests helps ensure the effectiveness of treatment and the health of both mother and baby. Treatment plans should be tailored to individual needs, and a collaborative approach involving obstetricians, hematologists, and other specialists is crucial. Postpartum management may involve continued anticoagulation therapy. Through comprehensive care and patient education, healthcare providers can optimize outcomes for pregnant women with APS.
Additional questions
- Is it possible for antiphospholipid syndrome patients to have a successful pregnancy?
Yes, patients with antiphospholipid syndrome (APS) can have a successful pregnancy with proper management and medical care. With early intervention, including the use of low-dose aspirin and heparin, along with close monitoring throughout pregnancy, the risks associated with APS can be significantly reduced.
- Is it possible to give birth naturally to antiphospholipid syndrome patients?
If the mother and baby are healthy during delivery, natural delivery is more likely to be successful. However, if the mother or baby is under stress or if the labor is premature, a cesarean may be the safest and fastest way to deliver.
- Which of the contraceptives is safe to use with APS?
Women with APS should avoid using contraceptives that contain estrogen, such as combined pills or the contraceptive patch. This is because estrogen can increase the risk of blood clots. If you have APS, it is safe to use these types of birth control:
- Mini pill (progesterone-only pill)
- Progesterone-only contraceptive injections
- Condoms
- What is the cause of frequent miscarriage?
Recurrent late miscarriage can be the result of uterine abnormalities, autoimmune problems, cervical incompetence, or premature birth.
- What is thrombocytopenia?
Thrombocytopenia is a condition that occurs when the platelet count in your blood is too low. Platelets are tiny blood cells made in the bone marrow from larger cells. When you are injured, platelets stick together to form a plug to seal your wound.
References
https://www.hss.edu/conditions_top-ten-antiphospholipid-syndrome-pregnancy.asp
https://www.tommys.org/pregnancy-information/pregnancy-complications/antiphospholipid-syndrome-aps
https://www.urmc.rochester.edu/encyclopedia/content.aspx?contenttypeid=90&contentid=p02432

