Many women experience ovarian pain from time to time; this is usually related to the menstrual cycle. The ovaries, located on either side of the pelvis, are responsible for producing and releasing the eggs needed for fertilization. Thus, the most common cause of ovarian pain, which is often felt in the lower abdomen, pelvis, or lower back, is related to ovulation and menstruation. However, gynecological problems such as endometriosis, pelvic inflammatory disease, or even a disease affecting the gastrointestinal tract or urinary tract can cause this pain.
Common causes of ovarian pain
The ovary is a small gland located on either side of the body and below the pelvic cavity of women. The ovaries are vital for reproduction and play an important role in the menstrual cycle and female sexual characteristics.
Each month, an ovarian follicle grows and becomes an egg. This process is called ovulation. In most women, this process is repeated regularly from the onset of puberty to menopause. Ovarian pain can occur in women during the menstrual cycle. The causes of this pain can be different.
Mittelschmerz
Some women experience ovarian pain during regular ovulation each month. This condition is called MittelSchmertz. The name is derived from the German words for “middle” and “pain.” Ovulation generally occurs in the middle of the menstrual cycle, so you will often feel pain around day 14 as the egg is released from the ovaries into the fallopian tube.
The unilateral or bilateral pelvis discomfort may be mild or severe and last from a few minutes to a few hours. Some women experience bleeding or discharge during ovulation, while others may experience nausea with pain. There are various theories as to why ovulation is associated with pain. One case is that the ovary has no cleft, so the egg must pass through the walls of the ovaries, which may cause damage.
Some doctors think that an enlarged egg in the ovaries just before ovulation can cause pain.
Mittschmartz pain usually resolves within a day and does not require treatment, although some women experience pain relief after starting birth control pills.
Ovarian cysts
An ovarian cyst is a benign sac that is usually full of fluid and may not cause pain, discomfort, bleeding, menstrual irregularities, or any symptoms. Ovarian cysts are common and can occur at different points during the menstrual cycle. Symptoms of ovarian cysts include pelvic pain, back, and thigh pain; other symptoms include:
- Pain during bowel movements
- Nausea
- Vomiting
- Breast tenderness
- Fullness in abdomen
- Pressure on bladder
- Frequent urination
There is a risk of rupture of the ovarian cyst if it enlarges. Symptoms of ovarian cyst rupture include:
- Sudden and severe abdominal pain
- Fever
- Vomiting
- Rupture of the cyst can also cause shock symptoms, including:
- Cold or clammy skin
- Rapid breathing
- Lightheadedness
Endometriosis

Endometriosis is a disorder in which tissue similar to the tissue lining the inner surface of the uterus grows outside the uterine cavity. The lining of the uterus is called the endometrium. Endometriosis occurs when endometrial tissue grows on the ovaries, intestines, and pelvic tissues. Expansion of endometrial tissue beyond the pelvic area is unusual but not impossible.
Hormonal changes in the menstrual cycle affect the abnormal growth of the endometrium, causing inflammation and pain in the affected area. Over time, the decomposed tissue has nowhere to go and gets stuck in the pelvis. The ovaries are often the area where endometriosis tissue grows and causes severe discomfort or pain. Other symptoms include:
- Painful periods, intercourse, or bowel movements
- Excessive bleeding
- Fatigue
- Diarrhea
- Constipation
- Nausea
The amount of pain felt may not be related to the degree of endometriosis. For example, a person may have severe pain but mild endometriosis.
Pelvic inflammatory disease
Pelvic inflammatory disease (PID) is an infection of the genitals and reproductive organs in women. The disease affects the uterus, fallopian tubes, and ovaries. This infection may occur naturally or be transmitted through intercourse. PID is more common in women between the ages of 15 and 25.PID may be symptomatic or asymptomatic. Symptoms may be mild or confused with conditions such as appendicitis, ectopic pregnancy, or ovarian cysts. PID may cause:
- Pain or tenderness in your pelvis
- Burning during urination
- Irregular bleeding
- Changes to vaginal discharge
- Pain during intercourse
- Fever
- Chills
- Nausea
- Vomiting
PID requires antibiotics to treat the underlying infection. Mild PID can be treated with one injection, while more severe PID may require a hospital stay for intravenous antibiotics.
Phantom pains
The ovaries are located near many different organs and parts of the body. As a result, pelvic and ovarian pain can be caused by other conditions.
Appendicitis
The appendix is a finger-like sac that protrudes from the large intestine on the lower right side of the abdomen, and appendicitis means inflammation of the sac. Appendicitis causes pain in the lower abdomen. However, in most people, the pain starts around the navel and then extends.
Constipation
Constipation is one of the most common digestive problems in the United States, affecting about 2.5 million people. This means that hard and dry defecation is done less than three times a week.
Kidney stones
Kidney pain can be severe on the side and back, near the ribs. There may also be blood in the urine, pain with fever, or chills.
Pregnancy
Delayed menstruation can be a sign of pregnancy. Other symptoms include chest tenderness, nausea, and vomiting, or fatigue. Ectopic pregnancy is another possibility if the pain is severe, especially in the shoulder and a light feeling in the head.
Urinary tract infection
If the pain is more in the center of the pelvis, it may be due to UTI. A urinary tract infection can cause frequent urination, a burning sensation when passing urine, or turbidity.
Ovarian remnant syndrome (ORS)
Sometimes the uterus must be removed during surgery for various reasons. When ovarian tissue inadvertently remains inside the pelvic cavity after an oophorectomy, it is called an Ovarian remnant. Bleeding during surgery, adhesions, anatomical changes, and even poor surgical technique can all cause ovarian tissue to remain. Pelvic pain is the most common symptom of ORS. After an oophorectomy, it is possible to feel a pelvic mass and not see the expected signs of menopause. Some women even have symptoms similar to those of endometriosis. Regardless, most women experience some symptoms in the first five years after surgery.
Torsion
The ovary is connected to the abdominal wall by a thin ligament through which the blood vessels and nerves that supply the ovaries also pass. That ligament may be twisted or even tied. If there is a cyst on the ovary, torsion is more common because the cyst causes the ovary to become heavier or larger than usual.
Uterine fibroids
Uterine fibroids are benign growths that arise from the lining of the uterus. In addition to pelvic discomfort or pressure, a woman with fibroids may experience abnormal uterine bleeding, back pain, constipation, urinary problems, and infertility.
Ovarian cancer
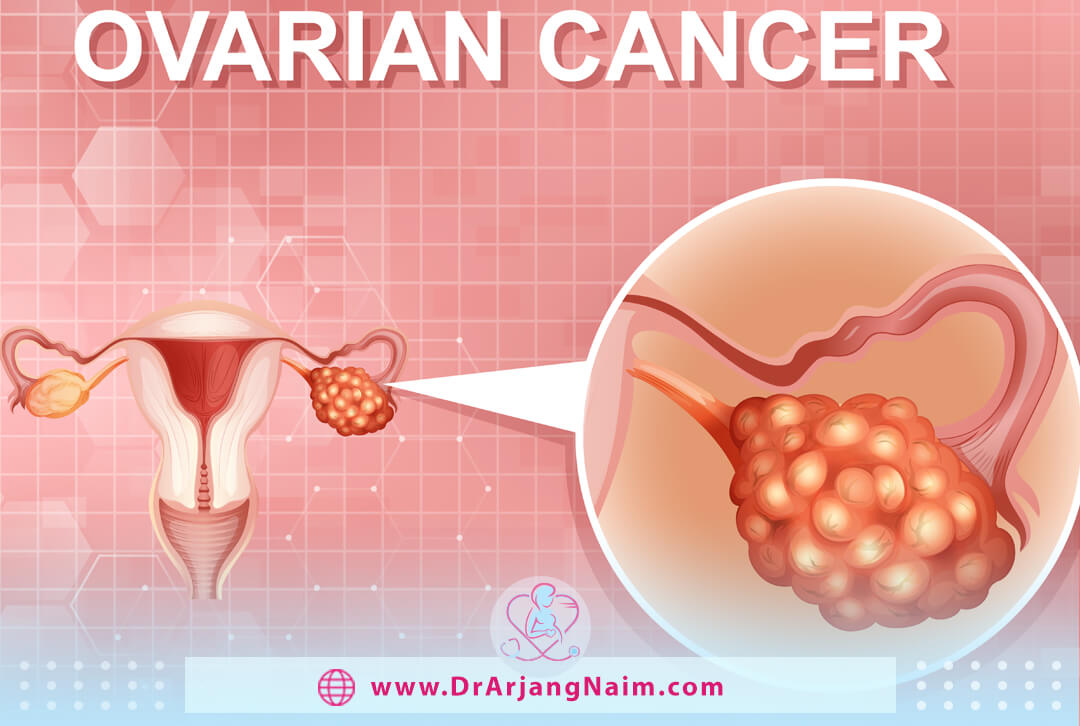
Although ovarian cancer can cause ovarian pain, it is not common. The disease often causes no symptoms or, if it does occur, more subtle symptoms such as bloating, feeling full without overeating, and urgency or frequent urination.
When to see a doctor
Whenever a woman experiences unusual pain in her pelvic area, she should consult a health care professional. The doctor may perform a pelvic exam or order additional diagnostic tests to help diagnose the source of the pain. Complications associated with ovarian pain depend on the cause of the discomfort. For example, there are no health problems or long-term problems with Mittelschmerz, but a ruptured appendix can be life-threatening if left untreated.
Untreated ovarian torsion can lead to ovarian death, loss of fertility, and even infection or severe death. The pain associated with ovarian torsion is usually very severe and causes a woman to need emergency medical help. Endometriosis or infections, such as PID, need to be treated to avoid other long-term problems such as infertility. Appendicitis or rupture of the ovarian cyst can cause infection or ulceration in the pelvis and can even be life-threatening if left untreated. Immediate medical attention is especially necessary if the pain is suddenly very severe or is accompanied by other symptoms.
Diagnosis
Diagnosing the cause of ovarian pain is not easy because problems with other genitals such as the uterus or cervix or even other body systems may be involved.
Medical and sexual history
Throughout the medical history, the physician asks the patient several questions about the pain, such as when the pain begins. What makes it better and worse are other symptoms such as vaginal bleeding, vaginal discharge, or fever. The doctor will also ask questions about a history of endometriosis or uterine fibroids and previous surgeries. The doctor also asks the patient questions about the number of sexual partners and sexually transmitted infections.
Physical examination
For ovarian pain, the doctor will examine the abdomen, lower back, and sides. In addition to inspecting and squeezing these areas for sensitivity, the doctor will also do a pelvic exam. During a pelvic exam, vaginal or cervical fluid samples may be taken through a Pap smear to check for infection or abnormal cells.
Imaging
Because there can be various reasons for the pain, the doctor may order imaging tests such as a pelvic ultrasound or a computed tomography (CT) scan of the abdomen and pelvis.
Labs and blood tests
Various tests may be prescribed to confirm or discount a diagnosis, perhaps the most important being a pregnancy test to rule out an ectopic pregnancy. In addition to a pregnancy test, a urine test may be done to check for blood or infection.
Pelvic laparoscopy
Pelvic laparoscopy is a surgery that is sometimes used to determine the cause of a woman’s pelvic pain.
Treatment
Once the cause of the pain has been determined, the patient and physician can design a treatment plan that may include a few lifestyle changes, such as taking prescription drugs or having surgery.
Lifestyle therapies
If ovarian pain is related to the menstrual cycle, lifestyle changes such as getting enough sleep, exercising, using relaxation techniques, and using a warm-up pad can often help relieve the pain.
Medications
Depending on the diagnosis, the doctor may recommend or prescribe medication. A nonsteroidal anti-inflammatory drug (NSAID), which lowers prostaglandin levels in the body, often helps. Another gynecological disease that requires medication is a pelvic inflammatory disease. If PID is diagnosed, the doctor will prescribe antibiotics.
Surgery
Surgery is necessary for emergencies, such as ovarian torsion or ectopic pregnancy. It is also often done as part of treating ovarian cancer, removing uterine fibroids or endometrial tissue in severe endometriosis.
The bottom line
Many women are not aware of the condition of their ovaries regularly. Meanwhile, many women suffer from ovarian cysts pain, or discomfort in these areas.
Even if ovarian pain does not interfere with daily activities, it is best to take action at the right time. Conditions such as endometriosis and PID can lead to infertility if left untreated. Appendicitis or rupture of the ovarian cyst can be fatal.
Arjang Naim, MD, helps the patient in diagnosis, examination of the pelvis, tests, and appropriate treatment to make the best decision for treatment by knowing the cause of the disease.
Additional questions
- Do cancerous ovarian cysts hurt?
When ovarian cysts cause symptoms, they can be similar to those of ovarian cancer. Common symptoms of ovarian cysts and ovarian cancer can include abdominal pain, bloating, pain during intercourse, menstrual irregularities, and rarely, frequent urination.
- What are the signs of early appendix?
Appendicitis pain often begins as mild cramping in the upper abdomen or navel that moves to the right side of the abdomen. Other symptoms associated with pain include:
- Loss of appetite
- Indigestion
- Nausea
- Vomiting
- Abdominal swelling
- Low-grade fever
- What are the signs of kidney stones?
Kidney stones usually do not cause symptoms until they move inside the kidney or into one of the ureters. If the kidney stone gets stuck in the ureters, it may block the flow of urine and cause swelling of the kidney and spasms of the ureter, which can very painful.
- Is a laparoscopy painful?
Laparoscopy is performed under general anesthesia, so no pain is felt during the procedure.
- How long is pelvic laparoscopy recovery?
Recovery from pelvic laparoscopy may take up to 6 weeks. If it’s a simple procedure like getting the tubal ligation, then two weeks is reasonable. For a laparoscopic hysterectomy, recovery may be closer to 6 weeks.
References:
https://www.healthline.com/health/womens-health/ovary-pain#ovarian-remnant-syndrome
https://www.verywellhealth.com/ovary-pain-causes-and-treatment-514437
https://www.medicalnewstoday.com/articles/320408#takeaway
https://ocrahope.org/2021/01/5-possible-causes-for-ovary-pain/
https://www.webmd.com/women/guide/ovarian-pain-causes-diagnosis-treatments

