Fetal distress, now called non-reassuring fetal status (NRFS), occurs when the baby in the womb does not show signs of well-being, usually due to insufficient oxygen. This can happen due to issues with the placenta, umbilical cord, maternal health, or complications during childbirth. Symptoms include changes in heart rate, decreased movement, or meconium in the amniotic fluid.
If you are pregnant and concerned about fetal distress, it is important to speak to your doctor or midwife straight away. They can monitor the health of your fetus and take action to fix any problems.
Signs of fetal distress
The main sign of fetal stress during pregnancy is the abnormal heartbeat of the fetus.
The following heart rate changes are signs of fetal distress:
- Tachycardia or fast heart rate above 100 beats per minute
- Bradycardia, or a slow heart rate of less than 60 beats per minute
- Variable decrease or sudden decrease in fetal heart rate
- Late slowing or gradual decrease in fetal heart rate after contraction
- Thick meconium in the amniotic fluid can also be a sign of fetal distress.
You should also watch out for these symptoms because they may cause discomfort to the fetus:
- Decreased, slowed, or no movement of your baby
- Severe cramping and severe back pain indicate complications
- Vaginal bleeding during pregnancy
- Rapid weight gain of more than 40 pounds
- Abnormality in the child’s breathing or movement in ultrasound
- Abnormal levels of amniotic fluid
Causes of fetal distress
There are several potential causes of fetal distress, which can be broadly categorized into issues affecting the following.
Placenta
- Placental insufficiency: This happens when the placenta does not function properly and prevents the delivery of oxygen and nutrients to the baby.
- Placental abruption: When the placenta partially or completely separates from the uterine wall, blood flow to the baby is cut off.
- Placenta previa: Abnormal implantation of the placenta on the cervix, potentially preventing the baby from coming out at birth.
Umbilical cord
- Prolapsed umbilical cord: When the umbilical cord descends into the vagina before the baby is born, it is likely to be compressed during labor.
- Umbilical cord entanglement: The umbilical cord wraps around the baby’s body, potentially restricting blood flow.
- True knot: A rare condition in which the umbilical cord knots itself and restricts blood flow.

Mother’s health
- High blood pressure: Preeclampsia and other conditions can limit blood flow to the placenta and baby.
- Infections: Some infections, such as chorioamnionitis, can inflame the placenta and harm the baby.
- Some medications: Some medications, such as blood pressure medications, may have side effects on the baby.
- Maternal health conditions: Chronic conditions such as diabetes or anemia can contribute to fetal distress.
Complications during childbirth
- Prolonged labor: When labor is too long, the baby may suffer from stress and lack of oxygen.
- Difficult delivery: Shoulder dystocia or other birth complications can restrict blood flow to the baby.
- Uterine Rupture: A rare but serious tear in the uterus can compromise the baby’s blood flow.
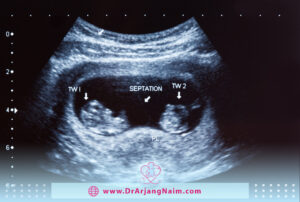
Fetal factors
- Multiple pregnancy: Twins or triplets are more prone to space and nutrient restrictions, potentially causing discomfort.
- Fetal growth restriction: If the baby is too small, it may not have enough reserves to handle stress.
- Birth defects: Some birth defects can affect a baby’s ability to receive oxygen or tolerate labor.
This list is not exhaustive, and any concerns about the health of the fetus should be discussed promptly with a healthcare professional. They can provide an accurate diagnosis and appropriate medical intervention when needed.
Diagnosis and tests
Your prenatal care provider can detect fetal distress by reading the fetal heart rate. A low heart rate or unusual heart rate patterns can indicate fetal distress.
The obstetrician-gynecologist may recommend other tests to monitor fetal heart rate during pregnancy.:
- Non-stress test: An electronic fetal monitor measures the fetal heart rate while sitting or lying down. A belt with an electronic sensor is placed around the abdomen. During this time, the fetus’s heart rate is measured and recorded. This test can also measure uterine contractions. The results are either reactive or non-reactive based on how active the fetus is.
Ultrasound biophysical characteristics measure fetal movement, muscle tone, respiratory movement, and amniotic fluid volume. Sometimes, it is combined with a non-stress test.
During labor, the obstetrician-gynecologist monitors the fetal heart rate continuously or intermittently. Continuous monitoring means wearing a device around your abdomen that reads the fetal heart rate. Intermittent monitoring means your doctor will check your baby’s heartbeat at times (such as every 30 minutes).
Two common ways to monitor fetal heart rate for fetal distress are:
- Electronic fetal heart rate monitor: During labor and delivery, you wear a device with a sensor attached to your abdomen. It sends the fetal heart sounds to a computer that the health care team can read.
- Doppler device: Gynecologists and obstetricians place a hand-held device on the abdomen that detects the fetus’s heartbeat using sound waves. Your obstetrician-gynecologist will use Doppler during pregnancy, most likely during your routine prenatal checkups.
Treatment
Treatment for fetal distress depends on the specific cause and severity of the situation. It’s crucial to remember that this information is for educational purposes only and should not replace professional medical advice. If you suspect fetal distress, always consult your doctor or midwife immediately.
Immediate actions
- Providing oxygen to the mother: This helps improve oxygen flow to the baby through the placenta.
- Administering fluids: Rehydration can support overall maternal and fetal well-being.
- Changing maternal position: Certain positions, like lying on the side, can improve blood flow to the uterus and placenta.
- Stopping medications that might be impacting the baby: This may include certain labor induction drugs.
Depending on the cause and severity
- Amnioinfusion: Introducing fluid into the amniotic sac can relieve cord compression and improve the baby’s environment.
- Medications: Medication to slow down contractions or improve blood flow might be used.
- Delivery: If the distress is severe or persists despite other interventions, the doctor may decide on delivering the baby, either vaginally or via cesarean section. This decision will be based on maternal health, gestational age, fetal well-being, and available resources.
Additional interventions
- Continuous fetal monitoring: Closely tracking the baby’s heart rate and other vital signs throughout the process.
- Ultrasound evaluation: Assessing the baby’s position, cord placement, and placental function.
- Cord blood sampling: Analyzing a small blood sample from the umbilical cord to assess fetal oxygen levels and acidity.
Remember
Early detection and intervention are crucial to improve outcomes for both mother and baby.
Treatment options will vary based on individual circumstances and should be guided by a qualified healthcare professional.
If you have concerns about your baby’s well-being, don’t hesitate to seek immediate medical attention. Please remember that this information is not a substitute for professional medical advice, and you should always consult your doctor for any questions or concerns.
Prevention
While there’s no guaranteed way to completely prevent fetal distress, many proactive measures can significantly reduce the risk.

Prenatal care
- Regular checkups: Attending all scheduled prenatal appointments allows for early detection and management of potential risk factors like preeclampsia, gestational diabetes, and infections.
- Healthy lifestyle: Maintaining a balanced diet, getting regular exercise (as approved by your doctor), and avoiding harmful substances like tobacco and alcohol all contribute to a healthy pregnancy environment for the baby.
- Weight management: Excessive weight gain or loss during pregnancy can pose risks, so aiming for healthy weight gain within the recommended range is crucial.
- Stress management: Chronic stress can negatively impact pregnancy, so incorporating relaxation techniques like yoga or meditation can be beneficial.
Monitoring fetal well-being
- Fetal movement tracking: Pay attention to your baby’s movement patterns and report any significant decrease to your doctor.
- Non-stress test (NST): This painless test measures the baby’s heart rate response to movement, providing reassurance about their well-being.
- Biophysical profile (BPP): Combining an NST with an ultrasound to assess fetal breathing, movement, muscle tone, and amniotic fluid level offers a more comprehensive picture.
Addressing health conditions
- Pre-existing conditions: If you have pre-existing medical conditions like diabetes or high blood pressure, managing them effectively with your doctor before and during pregnancy is essential.
- Infections: Promptly treat any infections that arise during pregnancy to minimize potential risks to the baby.
The bottom line
Obstetricians and gynecologists know how to recognize a child who is in distress during pregnancy and delivery. Listening to the fetal heart rate and paying attention to signs such as decreased movement are ways to recognize the unreliability of the fetus. Sometimes, the baby may be born early to avoid serious complications. Listening to your body and letting your doctor know about pregnancy and labor symptoms is the best thing you can do to reduce the risk of fetal distress.
Additional questions
- What are the long-term effects of fetal discomfort?
Fetal distress can have lasting effects on the child. A prolonged lack of oxygen during childbirth can lead to brain damage, cerebral palsy, or even stillbirth. If the baby is in distress, the provider will do everything possible to deliver safely before serious complications occur.
- What happens when there is meconium in the amniotic fluid?
Babies who are stressed due to low oxygen levels or infection may pass meconium before birth. When meconium enters the amniotic fluid, the baby may breathe it into the lungs before, during, or after birth.
- What is the difference between cord presentation and cord prolapse?
Both cord presentation and cord prolapse involve the umbilical cord being near the baby’s head during childbirth, but they differ crucially:
- Cord presentation: The cord is between the baby’s head and the cervix but inside the intact amniotic sac, usually not posing an immediate danger.
- Cord prolapses: The cord exits the cervix before the baby, with the amniotic sac ruptured, significantly increasing the risk of cord compression and requiring immediate action, often a cesarean section.
- What month does the baby’s heartbeat start?
The fetal heartbeat starts at the end of the fourth week of pregnancy. The heart, which begins to develop from the third week of pregnancy, has rapid and irregular contractions that can pump blood into the veins.
- Which medicine is harmful during pregnancy?
While it is impossible to list specific harmful medicines, remember that no drug is safe for pregnancy without consulting your doctor. Risks vary depending on the medicine, stage of pregnancy, and individual health. Always check with your doctor before taking anything, even over-the-counter or herbal remedies. They can provide personalized advice for your situation and a safe pregnancy journey.
References
https://www.medicinenet.com/what_are_signs_of_fetal_distress/article.htm
https://www.damoreinjurylaw.com/blog/fetal-distress/
https://my.clevelandclinic.org/health/diseases/23971-fetal-distress
https://patient.info/doctor/fetal-distress
https://www.whattoexpect.com/pregnancy/pregnancy-health/complications/fetal-distress.aspx

